When’s the last time you saw your doctor in person? For many people, that’s becoming a thing of the past, thanks to telemedicine services. As COVID-19 has forced all manner of gatherings from public spaces to virtual ones, it seems that medical care has not been left out.
What are telemedicine services? In short, it means meeting with your doctor or health care provider remotely, instead of in person. While some versions of telemedicine have been around since the 1950’s, new advances in technology such as video-conference apps and smartphones have made it easier for people to access.
Telemedicine services can consist of interactive, real-time communication between health care professionals and patients using phone or video conferencing; recorded messages that are sent between patient and care provider; or even remote patient monitoring, that uses mobile medical devices to collect diagnostic data.
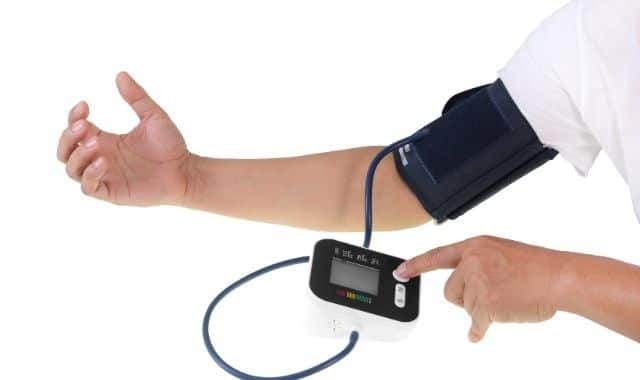
Telemedicine and e-health services have been hailed as a boon, and also criticized, for a variety of reasons.
Thanks to coronavirus risk management and physical distancing, telemedicine services are being widely expanded and used in many new ways. Doing away with physical exams in such a rapid and widespread way might be seen as highly experimental and controversial, if it weren’t for the current logistics challenges associated with the pandemic.
Those who are the most at risk for severe complications of COVID-19, such as elderly and immunocompromised individuals, can especially benefit from telemedicine visits, because they allow patients to avoid the additional exposure risk of waiting in a crowded waiting room with other ill patients.
Telemedicine visits are sometimes cheaper per treatment overall. Lowering the cost of health care benefits both patients and health insurance providers. Additionally, AI diagnostics and medical streaming devices allow physicians and nurses to provide more efficient care, while reducing the possibility of errors.
Telemedicine also does a great job of reducing the number of unnecessary doctor’s office visits, which saves consumers time and money. Another great benefit of telemedicine is that doctor’s visits can often be handled without the challenges of missing work, or scrambling to find childcare or eldercare in order to complete a visit.
While it’s clear that telemedicine is important, it’s also worth exploring how telemedicine is changing healthcare in profound and perhaps disconcerting ways.
First, there are barriers to telemedicine that we must contend with in order to continue accessing, and providing, quality health care. Not everyone has access to a personal device for telehealth visits, and new technology includes a learning curve that’s not always easy to master, especially in the elderly population.
There’s also many people who are concerned over the perceived impersonalization of health care, and telemedicine services may be blamed for accelerating that trend. Some health care providers believe that an increasing trend towards telemedicine will result in missed diagnoses, which may have long-term consequences.
Is telemedicine effective? For many health care professionals, that question is at the core of their decision to offer – or forgo – telemedicine visits in their own practice.
Dr. Paul Hyman, who has recently authored an essay in JAMA Internal Medicine, voices his concern that the “business of medicine has already started to devalue a doctor’s touch.” He shares that the pressure to see more patients per day results in spending less time with each of them.
Dr. Hyman already feels he has little time to actively listen to their concerns and answer their questions, and with telemedicine visits, his ability to read body language and pick up on vocal cues is also inhibited.
Like Dr. Hyman, many of us recognize that a major aspect of quality healthcare involves the physical touch, eye contact, and active listening that a patient and provider experience when they are fully present with one another. No AI or technology can fully replace that.
Finally, it’s important to consider that technology is expensive, and the health insurance industry moves slowly when it comes to implementing changes that align with common practice.
While 29 states currently have “telehealth parity laws” that require telehealth visits to be reimbursed in the same way as in-person medical treatment, this doesn’t necessarily mean that payments will be equal. The exact amount varies by insurance provider, and may only cover videoconference visits, but not other types of telemedicine services.
Regardless of these potential pitfalls, telemedicine is here to stay and we are all eager to see it improve rapidly.
Thankfully, as we see further advances in technology, billing and insurance standards, and medical providers integrating technology into their current practice, our experience of telemedicine services is likely to become even more positive in the near future.





0 Comments